Physiotherapy Of Shoulder Pain
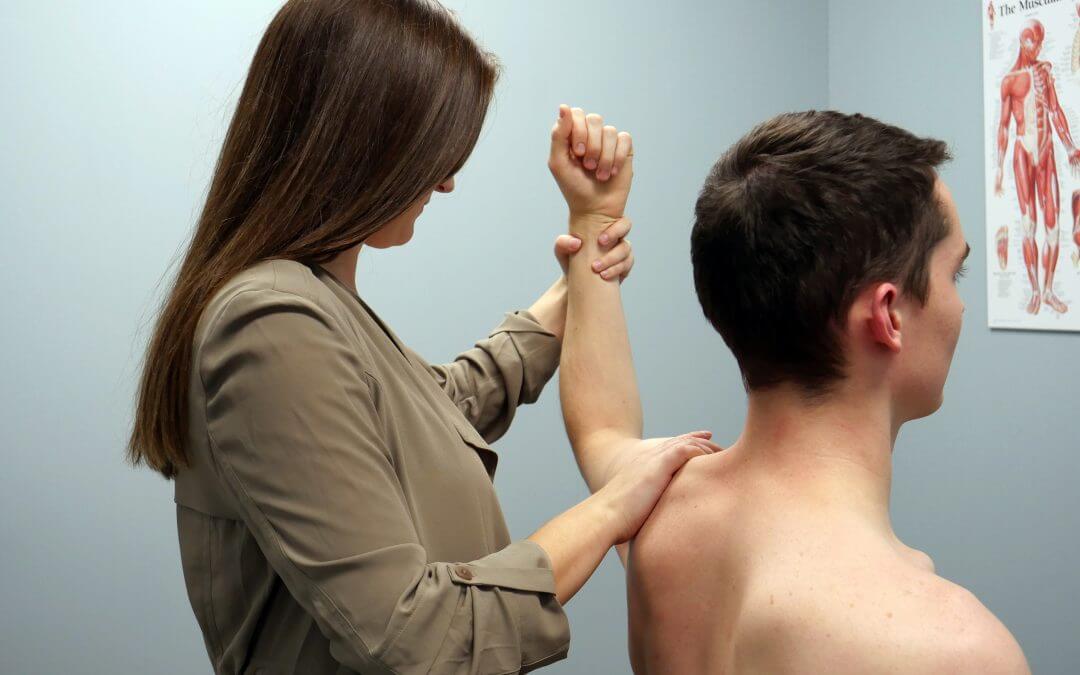
Abstract
Background: Shoulder disorders are a common condition in Australia. They have been found to affect anywhere from 7 to 36% of people (Lundberg 1969). This accounts for 1.2% (Bridges Webb 2012). Sheer shoulder disorders can lead to significant morbidity and substantial disability. There are many options for treating shoulder disorders. However, only a few treatments have been tested in controlled randomised trials. While physiotherapy is often considered the best treatment option for shoulder pain, evidence has not shown its efficacy. This review updates an earlier Cochrane study of shoulder disorders that included a review of various interventions.
Objectives: Determine the effectiveness of physiotherapy treatments for conditions resulting in stiffness, pain and/or disability at the shoulder.
Search strategy. From 1966 to June 2002, the Cochrane Clinical Trials Regiter was searched using MEDLINE, EMBASE or CINAHL. It was the Cochrane Musculoskeletal Review Group that used its search strategy. Keywords from past reviews as well all relevant articles were included in the text search.
There were two independent reviews that assessed the eligibility of each identified study for inclusion. For inclusion, the intervention had to be delivered generally by a physiotherapist and the allocation of treatment was randomly allocated. The study population must also have a shoulder disorder. This excludes trauma and other systemic inflammatory disease like rheumatoid.
Data collection and analysis Outcome data was extracted and entered into Revman 4.1. Means and standard deviations for continuous outcomes and number of events for binary outcomes were extracted where available from the published reports. All standard errors of a mean were converted into standard deviation. Additional details of trials were sought from first authors if the data required was not available or cannot be calculated. If there were no additional details provided, the trial was added to the review. The meta-analysis included all the information. Results were presented for each diagnostic sub group (rotator cuff disease, adhesive capsulitis, anterior instability etc) and, where possible, combined in meta-analysis to give a treatment effect across all trials.
Principal results: Twenty-six trials fulfilled inclusion criteria. There were many variables in the methodological quality. Also, trial populations were small. Median sample size 48. Range 14 to 180. Short-term rehabilitation in rotator ofcuff disorder was successful (RR 7.74 (1).97, 31.32) as well long term benefits in regard to functional ability (RR 2.45 (1).24, 4.86). For rotator Cuff Disease, exercise alone was more beneficial than mobilisation. It was found that laser therapy is more effective than placebo in adhesive capsulitis (RR 1.89, 7.288) but not in rotator-cuff tendinitis. The pain of calcific tendinitis was improved by both pulsed electromagnetic field and ultrasound (RR 1.81 (1), 2.60 (2) and RR 19, (1.16, 12.43), respectively). The effects of ultrasound on shoulder pain (mixed diagnose), adhesive capsulitis and rotator tendinitis are not supported. Although ultrasound has no added benefit to exercise, it is comparable with exercises. It is possible to show that corticosteroid injections can improve rotator cuff injury. But, there’s not much evidence that physiotherapy will be of any benefit to Adhesive Capsulitis. Reviewer’s Conclusions: There is very little general evidence regarding treatment due to small samples, inconsistent methodological quality, or heterogeneity between the population and the physiotherapy intervention used. Also, long follow-ups of randomised controlled trials of physiotherapy treatments have limited evidence. Some interventions can be used in limited cases. Trials of physiotherapy intervention for certain clinical conditions related to shoulder pain are needed. These include combinations of non-physiotherapy interventions and physiotherapy interventions. These trials are more representative of clinical practice. Trials must be properly powered and should address critical methodological criteria such blinding and allocation concealment of the outcome assessor.
Abstract
Scope: Shoulder pain can be a very common condition. Despite growing evidence of the importance of physiotherapy, in particular active exercise therapy, little data is available to guide treatment. The purpose of the project was to help develop an internationally recognized assessment and treatment method for patients suffering from shoulder pain.
Methods: A group of nine Swedish physiotherapists experienced in treating shoulder dysfunction met 2012 in Sweden in order to develop a treatment plan. To guide discussion, a questionnaire was filled out prior to the meeting. Virtual conferences allowed for the consensus to be reached.
Conclusions: A clinical reasoning algorithm that guides the treatment of patients who present with local shoulder pain without any significant passive range or instability was agreed upon. The algorithm stresses that treatment decisions for physiotherapy should not be based solely on structural pathology. That active exercises should be the first treatment method. A regular re-assessment should be done to make sure that any clinical aspects that contribute to the shoulder pain is addressed. The consensus was reached on the following guiding principles to implement exercise therapy for shoulders pain: a small number of exercises performed in a gradual manner, with proper scapulohumeral coordination.
Conclusion: This assessment and treatment method could be used to help establish an international consensus on a treatment plan for the shoulder pain.

Similar Articles
Effectiveness of individualized physiotherapy on pain and functioning compared to a standard exercise protocol in patients presenting with clinical signs of subacromial impingement syndrome. This was a randomized controlled trial.
Kromer TO, de Bie RA, Bastiaenen CH. Kromer TO, et al. BMC Musculoskelet Disord. 2010 Jun 9;11:114. doi: 10.1186/1471-2474-11-114. BMC Musculoskelet Disord. 2010. PMC free article. PMID: 2053414. Clinical Trial.
Efficacy and cost-effectiveness of a physiotherapy program for chronic rotator cuff pathology: a protocol for a randomised, double-blind, placebo-controlled trial.
Bennell K, Coburn S, Wee E, Green S, Harris A, Forbes A, Buchbinder R. Bennell K, et al. BMC Musculoskelet Disord. 2007 Aug 31;8:86. doi: 10.1186/1471-2474-8-86. BMC Musculoskelet Disord. 2007. PMC article free of charge Clinical Trial
Development and implementation of a physiotherapy intervention for use in a pragmatic randomized controlled trial in primary care for shoulder pain.
Dziedzic K, Stevenson K, Thomas E, Sim J, Hay E. Dziedzic K, et al. Musculoskeletal Care. 2009 Jun;7(2):67-77. doi: 10.1002/msc.151. Musculoskeletal Care. 2009. PMID 333407 Cervicothoracic Manual therapy Plus Exercise Therapy Versus Alone Exercise Therapy for Individuals with Shoulder pain: A Multicenter Randomized controlled Trial
Mintken PE, McDevitt AW, Cleland JA, Boyles RE, Beardslee AR, Burns SA, Haberl MD, Hinrichs LA, Michener LA. Mintken PE, et al. J Orthop Sports Phys Ther. 2016 Aug;46(8):617-28. doi: 10.2519/jospt.2016.6319. J Orthop Sports Phys Ther. 2016. PMID: 27477473 Clinical Trial.
An analysis of systematic reviews to determine the effectiveness of physiotherapy in treating musculoskeletal shoulder pain.
Chester R. Shepstone H. Daniell H. Sweeting D. Lewis J. Jerosch Herold C. Chester R. BMC Musculoskelet Disord. 2013 Jul 8;14:203. doi: 10.1186/1471-2474-14-203. BMC Musculoskelet Disord. 2013. PMC Article: Free PMID: 23834747 Review.
Background
All ages suffer from shoulder pain, and one-third of them are chronic. It is unknown what the most effective treatment might be. As a first treatment option, physiotherapy is frequently recommended. It is difficult to know from the initial assessment whether factors can predict how physiotherapy will be received by patients with shoulder pain. This study’s primary goal is to examine the relationship between shoulder pain and functional outcome six weeks after the treatment began.
Participating physiotherapy departments will recruit participants with shoulder pain musculoskeletal of all durations. The physiotherapist will determine the care path for this cohort study.
Potential prognostic variables will be collected from participants during their first physiotherapy appointment and will include demographic details, lifestyle, psychosocial factors, shoulder symptoms, general health, clinical examination, activity limitations and participation restrictions.
Six weeks after the start of physiotherapy, the outcome measures (Shoulder pain and Disability Index and Quick Disability of the Arm and Shoulder, Hand and Global Impression of Change), will be collected via postal questionnaires.
The treating physiotherapist may collect the details regarding attendance and treatment. Participants will need to do an exercise diet.
A first exploratory analysis of the potential prognostic factors will be done to determine their relationship at baseline. This is then followed by a multivariate statistical test. With a general linear approach, those factors with significant levels above 5% will also be taken into account as prognostic indicators.
An estimated 780 subjects provide greater than 90% power to detect an impact size of less 0.25, adjusted for variables that have a coefficient of determination R-squared. This could lead to an overall outcome of up to 0.5. 1000 participants would be first recruited, assuming that there will be a 22% drop in follow up after six months.
These studies may provide guidance for service users and providers to identify whether physiotherapy can be of any benefit. Some clinicians may offer guidance as to the key elements that will indicate whether physiotherapy is likely to be of benefit to patients.
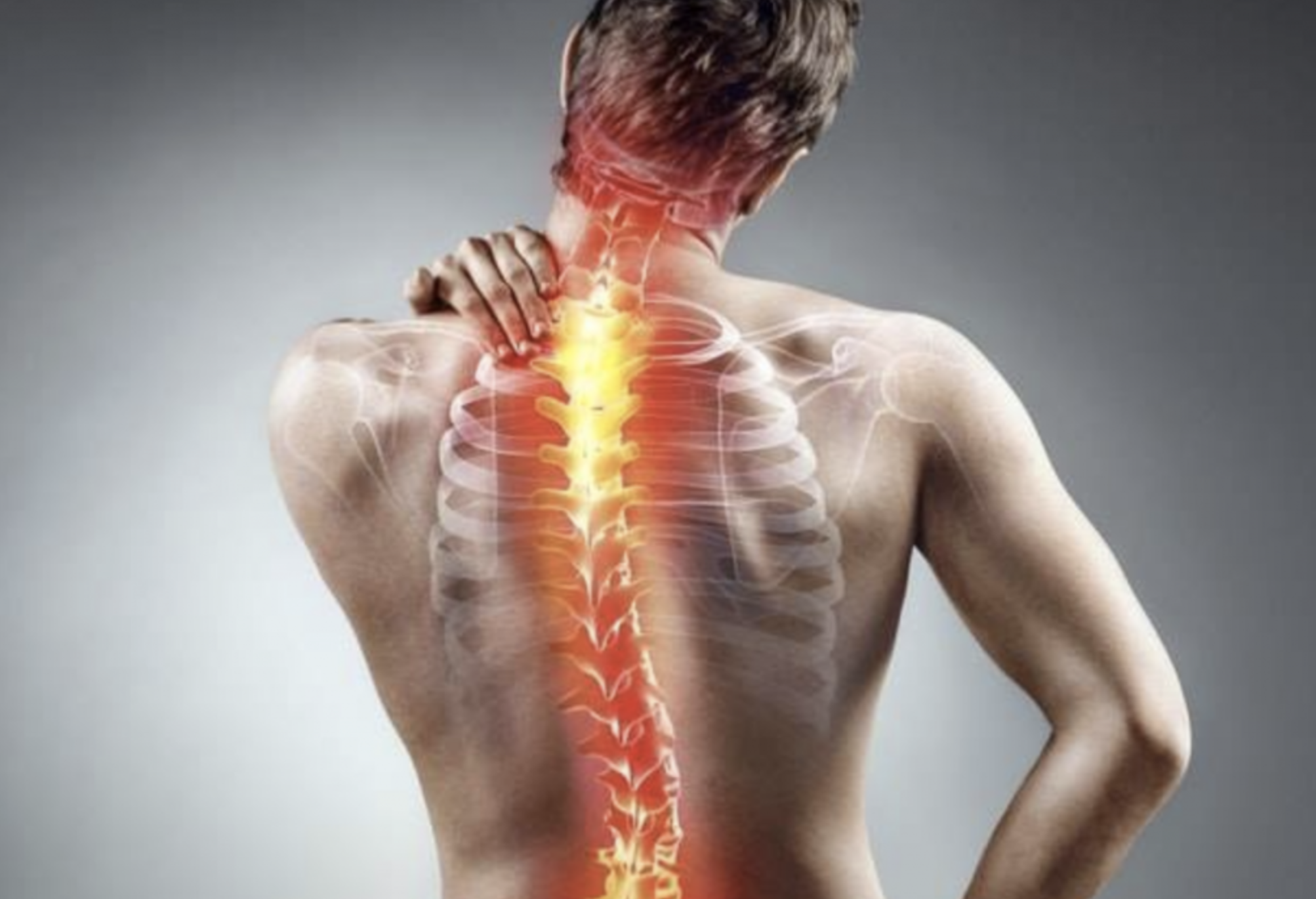
Background
There is an enduring musculoskeletal condition called shoulder pain. This problem affects everyone, and it can be a persistent, common, and sometimes permanent, problem. Shoulder pain is a common condition in the working population. It is not clear how much shoulder pain costs and what impact it has on the economy. According to both Swedish and Dutch studies, shoulder pain accounts for 50 to 84 percent of all healthcare expenses. Sickness absence due to shoulder pain in young working adults has been linked with high levels of sickness absence due to other diagnoses in subsequent years [ In primary care, shoulder pain is the third most common musculoskeletal presentation [ ]. Half of the people with shoulder pain who visited their general practitioners after experiencing their first episode were able to recover six months later. Only 10% of people who follow-up for one year show improvement in their recovery rates [ ]. It is still not known what the most effective treatment of musculoskeletal shoulder discomfort is. It is usually recommended that physiotherapy be used as the initial treatment. One third of the patients that are referred for physiotherapy or musculoskeletal ambulatory services in primary healthcare have severe shoulder pain. Although physiotherapy makes up a small percentage of overall healthcare cost, it accounts for approximately 37 to 60%. [When physiotherapy fails, pain management clinics and surgery may be considered. There is evidence to suggest that chronic pain is more likely for those with shoulder problems. It’s important to identify the right treatment early in the clinical journey, whenever possible.
It is currently impossible to predict which factors will influence the outcome of treatment for shoulder pain patients. Researchers have found that many biopsychosocial variables are linked to the outcome of shoulder pain management, whether it is under general or surgical care. This research aims at identifying the factors that influence shoulder pain outcomes following physiotherapy.
Patient care professionals, as well as commissioners, need to know more about prognostic factors to determine who might respond to physiotherapy. Other benefits include:
Enabling patients to make an informed choice about whether or not they wish to pursue physiotherapy based on the prognosis of a positive outcome.
Facilitating greater confidence and attendance in physiotherapy, which results in greater compliance.
Assisting physiotherapists to make timely decisions, and maximize resources.
To provide all health professionals with a tool for clinical reasoning to aid in distinguishing between those patients that respond to physiotherapy and those suffering from persistent symptoms.
Abstract
After treatment for mammary, pain and upper limb joint dysfunction are the most prevalent side effects. A prevalence range for these conditions was calculated for the USA. It varied between 12% and 51% regarding pain and between 1.5%- 50% concerning joint dysfunction. This research was conducted to determine if physiotherapy can be used for the treatment of shoulder pain caused by breast cancer.
A search was made on PubMed, Medline and CINAHL databases for pertinent publications from the past 10 years (1909-2019). All articles selected were based on correlation criteria. These included topics concerning shoulder pain in the aftermath of mammary tumors and any physiotherapy that was used to relieve this pain.
The treatment of musculoskeletal problems can be done by using active and passive exercises. Tissue mobilization, neurodynamics, accessory joint mobilization, and joint mobilisation are some examples. Both aerobic and strengthening exercises can be used to manage radio-induced or drug-induced neuropathic symptoms. These are done twice per week for approximately 150 minutes. To treat chronic pain effectively, multidisciplinary approaches are recommended. These include pain education intervention, pain pharmacological interventions (psychological interventions), and physiotherapy interventions.
To conclude. The classification of various types of shoulder pain in the aftermath of mammary carcinoma treatment requires targeted and specific physiotherapy intervention, where active therapeutic exercise is a major component.

Introduction
Breast cancer, the most frequent malignancy among women and leading cause of mortality and morbidity, is the number one killer. The world sees 1.67 Million new breast cancer cases every year. This is in addition to the 458,000 annual deaths from this disease [ ]. Side effects from breast cancer can last for many months, or even years. Only 89% of patients with the disease survive five years. The most common side effects are pain and joint dysfunction in the upper limb. This is determined by computing a range between 12.5% to 51% for pain, and 1.5% to 50% for joint dysfunction. [The study found that patients who have a lower Karnofsky performance status scale score and higher scores on the Social Communication Questionnaire had a greater chance of experiencing shoulder pain after treatment for mammary cancer. Furthermore, the patient’s poor general physical condition, low socioeconomic status, non-Caucasian race, and, finally, a low score on the Quality of Life scale increase this probability. The meta-analysis study indicates that the predictors of pain are the presence of preoperative shoulder pain and the younger age of patients [ ]. Many patients with mild to moderate pain are those who have had mastectomy and extensive, axillary resection. Patients suffering from this condition often have more lymph nodes or positive lymph nodes. Drains may also be inserted. In patients with moderate pain, there is an increased risk of complications.
Patients are often given an education booklet that includes a brief summary of advices and precautions. This is in addition to the preoperative assessment. McNeely’s study, in particular, suggests that a supervised rehabilitation intervention is preferable to the standard one, which instead uses an informative booklet, a written educational package, or unstructured or non-individualized exercises [ ]. By early identification and treatment of symptoms, customized physiotherapy is able to address complex issues related to postsurgical mammary tumor morbidity. The patient’s pain is the best indicator of the treatment that will be most effective. The causes of shoulder pain after treatment for mammary cancer include musculoskeletal pain type, radio-induced pain and drug-induced neuropathy. Breast cancer patients who have had their motor strategies reduced may experience a decrease in range of movements, which can lead to subacromial impingement, and consequently, more pain. Ebaugh stated in his study that pain due to postural instability, scar formation, or protection posture can result in a decrease of both the small and big pectoral muscles. This can lead to a depressed posture and an antepositioning effect on the shoulder. The misalignment could also be worsened by tissue fibrosis and radiation therapy. This would lead to an improper relationship between the scapula (and the chest wall) and between the hips and the glenoid fossa. These structural changes in the shoulder can eventually lead to pain.
You can divide neuropathic and drug-induced pain into three categories: neuropathy due to cancer; neuropathy caused by drugs, and neuropathy associated with the treatment of cancer. Common examples of neuropathic symptoms resulting from treatment for cancer include post-mastectomy discomfort syndrome. Neuropathic pain can also be caused by radiotherapy. In fact, radiotherapy can damage surrounding structures such as the nerves or the neural plexus. Finally, aromatase inhibitor drugs can induce neuropathic symptoms. This is the most common hormonal treatment used to treat hormone responsive tumors. It is manifested by arthralgia, osteoporosis, and the risk of fractures. As the leading cause of treatment suspension, arthromial symptoms are most common [ ]. Lipps’s analysis of radiotherapy side-effects [ ] analyzes the data. While radiotherapy may be an effective treatment for mammary tumors, it is not without risks. Some patients report side effects in the ipsilateral arm. Fatigue, skin reactions, and pain are the most frequently reported side effects; in particular, over 60% of patients experience pain at the end of treatment and, in 4% of cases, pain is reported to be severe or very severe. Radiation therapy of muscles and connective tissues within the shoulder joint can lead to the formation of fibrosis and atrophy and, therefore, to pain.
A staggering 50% of patients with chronic pain experience it six months after their surgery. The percentage of patients suffering from breast cancer with persistent symptoms is significantly greater than that of those without persistent breast pain and women who are not affected by it. A significant risk factor in chronic pain syndrome is poorly managed postoperatively. The 83% survival rate is not enough to explain why between 25% and 60% (or more) of all breast cancer survivors suffer from chronic pain. These persistent symptoms can result in a decreased quality of life and motor dysfunction. Certain patients who experience chronic pain are susceptible to central pain sensorization. This means that there is an increased risk of developing chronic pain.
.Physiotherapy Of Shoulder Pain
Kent Chiro-Med Wellness Clinic
| Website | https://www.kentchiromed.com/ |
| Address | 563 Gladstone Ave, Ottawa, ON K1R 5P2, Canada |
| Phone | +1 613-508-0113 |
| Category | Physiotherapy Ottawa |
Beverly Physiotherapy
| Website | http://www.beverlyphysiotherapy.com/ |
| Address | 747 Ellice Ave, Winnipeg, MB R3G 0B5, Canada |
| Phone | +1 204-774-8385 |
| Category | Physiotherapy Winnipeg |



















:fill(white)



