Percussion Chest Physiotherapy
Chest Percussion and Postural Drainage
To loosen and eliminate mucus in the lungs, postural drainage is often combined with chest percussion. The airway clearance procedures are useful for those who suffer from a spinal cord injury, cysticfibrosis, or any other condition that prevents mucus draining from their lungs. Lung infections can be worsened by mucus buildup.
Postural drainage relies on gravity to aid in the draining of mucus by placing the body into specific positions. The different positions of drainage affect the lobes (areas) in your lung. You can then spit out the mucus or exhale it.
The chest percussion or chest physiotherapy uses the vibration of the lungs to vibrate by clapping your chest and using a cupped hands. This vibration helps to transport the mucus into larger airways, which can then be coughed. The partner can help you vibrate your chest with special electronic devices that vibrate it.
These techniques should be performed as often as possible by a doctor or respiratory therapist. They need to be done every day, at minimum. These tasks should always be completed exactly as instructed.
Postural drainage can be done in the morning to clear up any mucus buildup from the night. It may reduce your nighttime coughing by performing postural drainage before you go to bed. Postural drainage should not be done soon after eating, as this could increase your chances of getting reflux.
Check out these photos to show you where to tap:
Postural drainage positions for children
Lower lobes (front) Lower lobes (sides) Upper lobes (back) Upper lobes (front)

Main Results
The search identified 157 research papers, out of which 8 cross-overs (data from 96 subjects) fulfilled the inclusion criteria. There was variation in the delivery of interventions between the studies, as many intervention groups combined multiple treatment methods. One study examined autogenic, six studies considered traditional chest physiotherapy and seven looked into oscillating positivatory pressure. Another included study examined high pressure positive expiredatory pressure. Of the eight studies, six were single-treatment studies and in two, the treatment intervention was performed over two consecutive days (once daily in one, twice daily in the other). A meta-analysis could not be done due to this heterogeneity. Blinding patients, caregivers, and clinicians in airway clearing studies is impossible. Accordingly this has not been considered to be a risk factor for bias. It was not possible to assess the risk of bias for many other criteria due to lack of protocol data.
A total of four studies involving 28 patients found that expectorated secretions were higher during chest physiotherapy than in a placebo. An 18 participant study found no difference in sputum size. In five studies radioactive tracer clearance was used as an outcome variable. It was found that radioactive tracer levels were higher in the treatment period for chest physiotherapy than it was during control. One participant in the 12-person study noted an increased radioactive trail clearance with all interventions. This was not reported for postural drainage, vibrations, or percussion. And the other eight participants reported that there wasn’t any difference between chest physiotherapy with coughing and radioactivetracer clearance with the treatment. Three studies, involving 42 participants reported no significant effect on pulmonary function variables following intervention; but one further study did report significant improvement in pulmonary function following the intervention in some of the treatment groups.
Results of the review showed that airway clearance techniques are short-term in their ability to increase mucus transport. Unfortunately, no data was available to make long-term conclusions.
Abstract
Introduction: Chest physiotherapy (CPT) may benefit children aged < 5 years who suffer from lower respiratory tract infection (LRTI). However, its effects are technique-dependent. In this study, we compared manual and mechanical CPT among children with LRTI.
Methods: Children aged 5 months to 5 years who were admitted and referred for CPT from January to April 2017 were randomised to either manual CPT or mechanical CPT with LEGA-Kid(r). Pre-intervention and two hours later, outcomes were measured as respiratory rate (RR), oxygen saturation, and modified Respiratory Dystress Assessment Index (mRDAI).
Results: After intervention, all 30 patients enrolled had significant decreases in their mRDAI and RR scores. There was an 8% reduction in RR for the manual CPT group (p = 0.002) and a 16.5% reduction in the mechanical CPT group (p = 0.0001), with a significantly greater reduction in the latter (p = 0.024). mRDAI scores dropped by 2.96 for the manual group (p 0.0001) and 3.62 for the mechanical group (p 0.002); there was no statistically significant difference among the two groups. CPT didn’t show any significant increase in oxygen saturation. There were no adverse events.
Conclusion: Children receiving either manual or mechanical CPT showed improvements in respiratory distress symptoms with no adverse effects. The combination strategy that includes nebulised hypotonic saline and CPT to LRTI reduces the severity of severe respiratory distress. The LEGAKid mechanical CPT technique was more effective in decreasing RR.
Keywords; children; lower respiratory tract infection; manual chest physical therapy; mechanical percussor.

Abstract
The treatment of breathing conditions has long used manual chest physiotherapy (MCP), which involves vibration, shaking, and chest percussion. Because of limitations in research methods, this method has not been widely used. In patients suffering from an exacerbation (or worsening) of Chronic Obstructivepulmonary Disease, the clinician will decide whether to give MCP to help with sputum drainage. We evaluated the effectiveness of MCP in assessing its impact on disease-specific quality and life.
Five26 people with severe COPD were included in this controlled, randomised trial. The four UK hospitals where they were located enrolled them. Patients received MCP and advice either on their airway or on their chest. The primary outcome was a COPD specific quality of life measure, the Saint Georges Respiratory Questionnaire (SGRQ) at six months post randomisation. The intention to treat (ITT) was used for analyses. ISRCTN13825248 registered it.
All patients participated in analyses. 372 of them (71%) gave evaluable information for the primary outcome. To determine superiority, the effect size was 0*3 standard deviations from SGRQ scores. ITT analyses revealed no statistically significant differences in SGRQ scores for patients who had or did not get MCP (95%CI -0*14 – 0*19).
These data support MCP routinely in COPD treatment for acute COPD exacerbations. This does not necessarily mean MCP has no therapeutic value for COPD patients under certain circumstances.
Chest Physiotherapy
Andrea R. Levine Jason Stankiewicz. Click Here for Patient Education. Chestphysiotherapy involves external mechanical maneuvers (such as chest percussion or postural draining) to improve mobilization, clearance, and mobilisation of airway secretions. For patients with a persistent cough that is not able to clear dense, sticky, bulky, or located secretions, it is recommended. This is recommended… Read more Bronchiectasis Bronchiectasis Bronchiectasis refers to the inflammation and dilation of the larger bronchi. There are many causes, including cystic fibrosis (also known as immune defects) and persistent infections. Alpha-1 antitrypsin deficiencies and occupational…read more can cause chronic obstructive lung disease (COPD) in some clinical circumstances (General References). Chest physiotherapy uses external mechanical techniques such as vibrations, chest percussions and postural drainage to enhance mobilization and clear out airway secretions. It’s indicated… read More Cystic fibrosis Cystic Fibrosis, an inherited disorder of the exocrine cells that affects primarily the respiratory system and the digestive. It leads to chronic lung disease, exocrine pancreatic insufficiency… read more Neuromuscular disorders Pneumonias Overview of Pneumonia Pneumonia is acute inflammation of the lungs caused by infection. Chest xrays and other clinical findings are often used for diagnosis. The causes, symptoms, treatment and preventive steps are all determined in the dependent lung areas. Despite the lack of high quality clinical trials that provide strong evidence-based support for cystic fibrosis, chest physiotherapy is still an essential component of patient care. Cystic Fibrosis is an exocrine disease which affects the respiratory and gastrointestinal systems. It leads to chronic lung disease, exocrine pancreatic insufficiency… read more
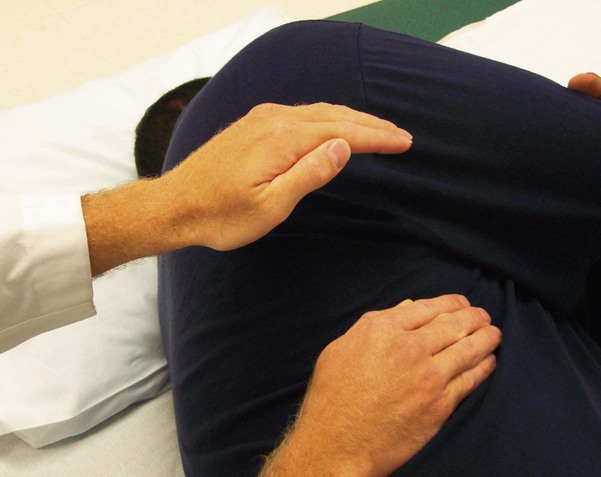
Procedure
A respiratory therapist may administer chest physiotherapy, but the techniques are often taught to loved ones of patients.
Postural draining and chest pressing are the most used. With postural and chest compression, the patient’s chest is turned to permit drainage. Also, retained secretions can be loosened and mobilized by being held with cupped hands. This procedure can prove to be uncomfortable and exhausting. There are other options to hand chest percussion, such as mechanical vibrators or inflatable vests.
There are other ways to clear the airways. These include controlled breathing patterns, positive exhalatory pressure devices for maintaining airway patency, ultra-low-frequency airway oscillations to mobilize stool, and controlled patterns of breath. Airway clearing methods are similar, so it is important to choose the right method for you.
What’s chest physiotherapy?
CPT, or chest physiotherapy is an effective way to remove mucus from your lungs. The lobes of the lungs, both back and front, are shown below.
CPT includes bronchial and percussion. Learn CPT from a Respiratory Therapist.
Bronchial drainage (BD) is positioning the body to allow gravity to help in moving the mucus. The area that needs to be drained can vary depending on the position.
Percussion, also known as clapping, involves tapping your chest rhythmically in order to release mucus from the bronchial tubes.
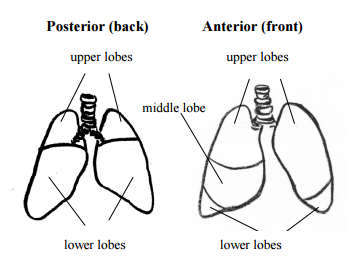
Use these pointers to help you practice
Chest physiotherapy includes a variety of techniques, such as conventional chest physiotherapy (i.e., percussion and postural drainage), active cycle of breathing techniques, positive expiratory pressure (using devices to maintain 10 to 25 cm of water pressure during expiration), and osteopathic manipulation. These methods could theoretically help maintain open airways and enhance gas exchange. Results from previous studies have been mixed, and there were no previous systematic reviews.
In the Cochrane Review, six studies were found that evaluated chest physiotherapy in adults suffering from acute pneumonia. Seven additional studies did not appear to fit their inclusion criteria. They excluded five that were published in Russian, one which had not been published, and one that was in 1947. The remaining one, however, was unavailable to them. The included studies had all been randomized. Three of them blinded the participants and two of them blinded the outcome assessors. There was also a concealed allocation. All patients received standard treatment, such as antibiotics or oxygen therapy. Two studies compared additional chest physiotherapy with placebo therapy, while four others compared no therapy, i.e., only routine treatment, in all of them. None of the interventions improved mortality or cure rate. In two double-blinded, controlled trials, osteopathy manipulation was tested with 79 patients. It appeared that it reduced the hospital stay length by one day and prolonged antibiotic therapy.
Register or pay for access to see the complete article
MARK H. EBELL, MD, MS Author Disclosure: Dr. Ebell serves as Editor in Chief for Essential Evidence, which is published by John Wiley & Sons, Inc., and The Cochrane Library.
.Percussion Chest Physiotherapy
Kent Chiro-Med Wellness Clinic
| Website | https://www.kentchiromed.com/ |
| Address | 563 Gladstone Ave, Ottawa, ON K1R 5P2, Canada |
| Phone | +1 613-508-0113 |
| Category | Physiotherapy Ottawa |
Beverly Physiotherapy
| Website | http://www.beverlyphysiotherapy.com/ |
| Address | 747 Ellice Ave, Winnipeg, MB R3G 0B5, Canada |
| Phone | +1 204-774-8385 |
| Category | Physiotherapy Winnipeg |



















:fill(white)



