Chest Physiotherapy Techniques

Abstract
Background: Cystic fibris is a genetic life-limiting condition that can be inherited. It’s characterised by thick, persistent airway secretions and pulmonary infections. In order to facilitate the removal of secretions, chest physiotherapy is an integral part of clinical management. While traditional techniques of chest physiotherapy (CCPT), required assistance, more modern techniques to clear airways can be done by the user. They are easier and more flexible.
Objectives: To assess CCPT’s effect on breathing, individual preferences and quality of life.
Search strategy. CINAHL (1982 to 2002) and AMED (1985-1902) were also searched. The date of the most recent search was January 2004.
Criteria for selection: Randomised, quasi-randomised clinical trials. This includes those that used CCPT in comparison to other airway clearing techniques. Study durations of less seven days were exempt.
Data collection and analysis: Two reviewers allocated quality scores to relevant studies and independently extracted data. In the event that we could not extract data, authors were invited to provide their data. Meta-analysis was not performed on studies whose data had been lost or when study design prohibited comparison. The generic inverse variance technique was used to meta-analyze data from crossover trials. Parallel-designed data were also used for comparison. Additionally, we evaluated the effectiveness of particular techniques as well as effects on treatment duration.
Main results: Seventy-eight publications were identified by the searches. Twenty-nine of these were included, representing 15 data sets with 475 participants. In terms of lung function measurements, there were no major differences in the results between CCPT (or other airway-clearance techniques) and CCPT. No matter what airway clearance technique was used, studies conducted during acute exacerbations revealed significant increases in respiratory function. Longer-term studies demonstrated smaller improvements or deterioration over time. Ten studies reported individual preferences for technique, with participants tending to favour self-administered techniques. This data could not be used for meta-analysis because of heterogeneity in preferences measurement.
Authors’ conclusions: This review demonstrated no advantage of CCPT over other airway clearance techniques in terms of respiratory function. There was a trend for participants to prefer self-administered airway clearance techniques. There were a few short-term studies that weren’t well designed and sufficiently powered.
What’s chest physiotherapy?
The practice of chest physiotherapy, which focuses on physical techniques to improve the function of your lungs and make it easier for you to breath better, is known as chest therapy. CPT (Chest Physical Therapy) is a form of chest physiotherapy. CPT strengthens breathing muscles, expands the lung, and reduces or eliminates thickening and swelling in the lungs. Cystic Fibrosis, COPD (chronic Obstructive Pulmonary Disease) are two examples of conditions that chest PT treats. The lungs are kept clear during immobility and after surgery to avoid pneumonia.
There are many ways to manage respiratory conditions. Chest physiotherapy can be used as one option. Before you have chest physiotherapy, get a second opinion.
Chest percussion and vibration to help loosen lung secretions. Some patients wear a special CPT vest hooked up to a machine. In order to dissolve the secretions in the body, the machine causes the vest vibration at high speed.
Controlled coughing techniques to help break up lung secretions so your caregiver can suction them out or you can cough them up.
You can deep breathe to increase lung capacity and expand the lungs. After surgery, you can use the device to help reexpand your lungs.
Turning from one side or the other can help to increase lung expansion. For patients in hospital or bedridden, this is crucial.
For the drainage of lung secretions, postural drainage may be done. Doctors will recommend other treatment options to address respiratory problems and improve breathing. The treatment options available depend on what type of disease you have, how severe it is, your medical history and your age. Some of the procedures for chest PT include:

What are the potential risks and complications of Chest Physiotherapy treatment?
When the technique is appropriate to each patient, chest physiotherapy can be safe. There are some complications that chest physiotherapy could cause, for example, if the head is being lowered.
Chest physiotherapy should be avoided for people with the following conditions:
A decrease in blood flow from anticoagulants or blood thinners. Open wounds that are not closed. Pain, dizziness, fatigue, nausea and shortness of breath are some symptoms. Also, it is important that you follow your treatment plan. This includes taking medication and using breathing therapies as instructed.
How Do I Prepare For Chest Physiotherapy?
Your comfort level and the outcome of chest physiotherapy are affected by what you do before it begins.
Do not eat before you have chest PT. In order to reduce sputum buildup, you may need to drink at least one glass of water. A doctor, nurse, and respiratory therapist might give additional directions before doing chest PT.
A list of questions you can ask your doctor or nurse. Sometimes patients forget about some details regarding their illness and treatments. It is possible to think of additional questions later on, after you’ve left the hospital. Contact your doctor with concerns and questions before chest physiotherapy and between appointments.
It is a good idea to bring a list of questions to your appointments. Common questions include:
Why do I need chest physiotherapy? Is there another treatment option?
Do I have to go to chest physiotherapy as often as possible?
What should I do to take my medication?
What time should I follow-up with you?
Do you have a contact number? Get numbers that you can reach during normal business hours and at night.

What are my options after chest physiotherapy treatment?
It is difficult work to do chest PT. However, your ability to tolerate the therapy more will increase as you improve. If you feel tired or uncomfortable, tell your provider. The techniques can then be modified. You can breathe more easily, get more oxygen to your blood and have a better quality of life with chest physiotherapy.
View All Breathing, Lungs and Respiration Articles
This tool is not intended to provide any medical advice. It is intended for informational purposes only. It cannot be used to substitute professional medical advice. Do not disregard the advice of professional doctors when seeking treatment due to something you read. Do not hesitate to call 911 or your doctor if it appears that you are in a medical emergency.
Chest physiotherapy (CPT). Nursing reviews.
Trendelenberg can be used to treat chest pain. Children’s Hospitals and Clinics of Minnesota
Chest Physiotherapy Treatment (CPT). Cincinnati Children’s Hospital Medical Center.
High-Frequency Chest Wall Oscillation (the Vest). Cystic Fibrosis Foundation.
Welcome To Our Patient Education Page!
A team of specialists and staff believes that informed patients will be better equipped to make health-related decisions. For your personal use, we have created an extensive patient library covering an array of educational topics, which can be found on the side of each page. These diagnoses and treatments will help you learn about your interests. Or, for a more comprehensive search of our entire website, enter your term(s) in the search bar provided below.
Please feel free to contact our office with any questions.
A variety of physical methods are used to clear mucus out of the respiratory passages, improve breathing, and help with chest physiotherapy. The goal is to help patients breathe more freely and get more oxygen through the blood stream into all parts of the body.
Normal mucus acts as a lubricant for the lungs. But infection, trauma or illness can create excess mucus that needs to be cleared for better breathing. These methods are often used by respiratory therapists, physical therapists, and other professionals who work with people suffering from:
From Chronic Obstructive Pulmonary disease (COPD)

The Safety and Efficacy of Chest Physiotherapy in Patients with Covid-19: An Inquiry
1 Department of Physiotherapy Bayero University Kano Kano Nigeria
2 Department of Physiotherapy and Rehabilitation Sciences University of Antwerp Antwerp Belgium
COVID-19, the current global pandemic, has caused a worldwide famine that has resulted in death and morbidity. In these cases, pneumonia and respiratory disease are two of the leading causes of death. A technique that can improve gas exchange is chest therapy. If it is given very early in respiratory problems, this may reduce the need for artificial ventilators. There is little evidence of its effectiveness in COVID-19 patients, particularly in acute stages and for patients who are on ventilators. However, patients discharged from hospital after COVID-19 have seen improvements in their FEV1 and FVC, FEV1/FVC% and endurance. They also experienced a decrease in depression and anxiety symptoms. The question of whether or not chest physiotherapy has the ability to disperse the aerosols, accelerate spread and speed up the spread is still open. Some believe it is possible. Other authors feel that the range of aerosols generated by chest-physiotherapy is dangerous. For cross-infection prevention, you can use self-management tools and surgical masks.
Introduction
Coronavirus 2019(COVID-19), also called SARS COV-2 in recent years, is a coronavirus. The virus is transmitted via droplets to large extent ( ). When one contracts the infection, the virus gets into the lungs and is received by angiotensin-converting enzyme 2 (ACE2), which is expressed in normal humans in types I and II alveolar cells ( ). The virus binds to ACE2 in the alveolar cells. The alveolar cells function under normal circumstances to synthesize and secrete surfactant, carry out xenobiotic metabolism, help with transepithelial movement of water, and regenerate alveolar epithelium following lung injury ( ). The functions mentioned above are important for maintaining normal lung functions. In other words, respiratory problems or systemic manifestations can result from damage to the alveolar tissues ( ). Consequently, clinical manifestations of COVID-19 disease include fever, cough, myalgia or fatigue, pneuomia, and complicated dyspnea ( In addition, when the respiratory symptoms are severe, they may progress to respiratory failure (acute respiratory distress syndrome), which could lead to death unless it is managed promptly using invasive ventilation ( ). For mild-to-moderate symptoms, chest physiotherapy is an alternative treatment (). This article will critically examine the causes of COVID-19-related respiratory issues in COVID-19 patients and discuss the safety and effectiveness of using chest physiotherapy. PubMed was searched with COVID-19 as the keywords, while Google Scholar used pulmonary rehabilitation and chest physiotherapy.
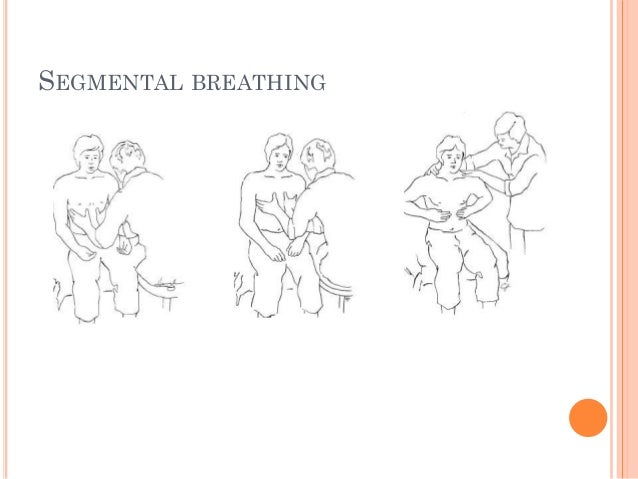
Chest Physiotherapy During Mechanical Ventilation
The patient may not be able to breathe spontaneously if they are under mechanical ventilation. This can predispose the patients to developing lung collapse and ventilator-associated pneumonia. In such circumstances, chest physiotherapy can be used to reduce the length of stay in both a mechanical ventilator and ICU and prevent ventilator-associated pneumonia ( ). The high-frequency, chest wall oscillation of intubated patients also resulted in an increase in dry sputum weight (PaO) on day three and decreased lung collapse in days 2 and 3. On day 3, culture positivity improved on day 3 (). Another patient had 11 sessions in physical therapy. These included exercise, mobilisation, upright body posture, breathing, and active cycling of breathing techniques every 2 hours for 12 hrs during his 48-hour ICU stay. Six sessions were on day 1 and five on day 2. The arterial oxygen level also improved with radiographic resolution. Since chest physiotherapy can reverse pathological progression and prevent atelectasis as well as improving impaired gas exchange and decreasing culture positivity (which are some of the hallmarks of COVID-19), it is possible to be used in patients suffering from this condition.
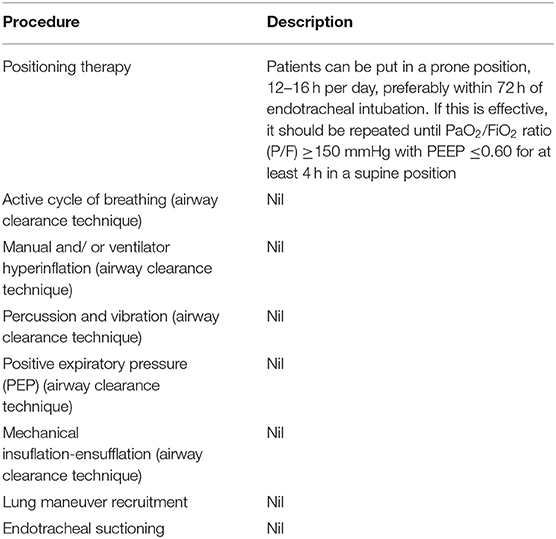
The following techniques are recommended for patients on ventilators: endotracheal suctioning ( ), lung maneuver recruitment ( ), and airway clearance techniques. The airway clearance techniques recommended include positioning, active cycle of breathing, manual and/or ventilator hyperinflation, percussion and vibration, positive expiratory pressure (PEP), and mechanical insuflation-ensufflation ( ). The details of how to use these techniques, aside from the positioning therapy, are unclear. There have not been studies in COVID-19 patients that report on their efficacy. You can see the details in Table 1 about positioning therapy. In addition, lung maneuver recruitment needs to be used with caution since it may have severe adverse effects ( ). Also, the state of the patients’ respiratory, cardiovascular and neurological systems will determine whether chest physiotherapy should be performed during this period. Refer to Table 2 for information about contraindications.
Which are the 3 techniques used in chest physiotherapy treatment?
Chest physical therapy (CPT or Chest PT) is an airway clearance technique (ACT) to drain the lungs, and may include percussion (clapping), vibration, deep breathing, and huffing or coughing.
Which Technique Is The Most Effective For Chest Physiotherapy?
Therefore, chest physiotherapy should be administered routinely two times per day. This frequency is increased during bronchitis flare-ups. The most frequently prescribed treatment is postural and percussion drainage.
What are The Steps of Chest Physiotherapy Therapy?
Chest physical therapy (CPT) is a technique for airway clearance in order to drain the lungs. The treatment involves vibration (clapping), breathing, breathing, and coughing.
What Are Physiotherapy Techniques To Clear Serums?
Respiratory physiotherapists can use percussion to enhance airway clearing by mobilizing secretions within one or more segments of the lungs to the central arteries. Percussion over an affected area produces an energy wave, which is transmitted to the lungs and airways.
.Chest Physiotherapy Techniques
Kent Chiro-Med Wellness Clinic
| Website | https://www.kentchiromed.com/ |
| Address | 563 Gladstone Ave, Ottawa, ON K1R 5P2, Canada |
| Phone | +1 613-508-0113 |
| Category | Physiotherapy Ottawa |
Beverly Physiotherapy
| Website | http://www.beverlyphysiotherapy.com/ |
| Address | 747 Ellice Ave, Winnipeg, MB R3G 0B5, Canada |
| Phone | +1 204-774-8385 |
| Category | Physiotherapy Winnipeg |



















:fill(white)



